Muscle Loss Is Not Just Aging, It Is Biology You Can Influence
Peer Reviewed by Dr. Scott Rollo, PhD and Dr. Peter Rawlek, MD
Many people assume losing muscle as we age is simply part of getting older.
But the science shows something different. Muscle loss, called sarcopenia, is a biological process that often begins to accelerate in our 40s. The encouraging news is that it responds strongly to the signals we send our bodies through daily movement.
Muscle decline is not random
Several forces quietly drive muscle loss over time. Hormonal changes. Chronic low level inflammation. Long periods of sitting. Poor nutrition. Genetics also plays a role.
These factors slowly change how muscle cells behave. Over many years, they shift the body toward losing more muscle than it rebuilds.
But this process does not happen overnight. It develops gradually and can be influenced by how we live.
The nervous system is part of the story
Muscles do not work alone. They depend on signals from nerves.
With age, some of the nerve cells that control muscle fibers slowly decline and die off, especially with lack of use. By the seventh decade of life, roughly half of the motor neurons that once activated muscle may be lost, but this step wise decline starts in mid life (40s). When this happens, muscle fibers shrink and stop functioning.
This is why strength, balance, and coordination can decline if muscles and nerves are not regularly challenged.
Movement helps maintain these critical connections. With more exercise, more active nerves are stimulated, more nerve connections, and then, more muscle.
Changes are also happening inside muscle cells
Inside the muscle, repair systems gradually slow down and they slow down quicker when there are low levels of regular activity.
Special repair cells called satellite cells become less active. Protein building slows. Some muscle proteins break down faster than they are rebuilt. Fat then slowly accumulates replacing muscle tissue.
These changes affect the fast twitch muscle fibers that help us move quickly, climb stairs, or catch ourselves if we trip.
Over time this leads to less muscle mass, reduced strength, and higher risk of falls or injury.
But again, this process is not inevitable.
Inflammation is one of the hidden drivers
Research now shows that chronic low level inflammation plays an important role in muscle aging.
Inflammatory molecules called cytokines, [common ones are TNF alpha, IL 1 beta, and IL 6] interfere with muscle repair and muscle protein production. These signals increase when you spend long periods sedentary, eat highly processed diets, and avoid regular physical activity.
In simple terms, inactivity creates an environment that slowly pushes muscle toward decline.
Movement does the opposite.
Exercise changes the biology of muscle
Exercise is one of the most powerful signals the body can receive.
Resistance training, such as bodyweight exercises, bands, or weights, tells the body to build and protect muscle tissue. It increases muscle protein synthesis and improves muscle strength and quality.
Aerobic activity, such as walking, cycling, or swimming, works in a different way. It improves circulation, increases oxygen delivery, reduces excess body fat, and lowers systemic inflammation.
Aerobic exercise also helps regulate important cellular signals that support muscle repair and regeneration.
Both types of activity are working on the same problem from different directions.
Movement also calms inflammation
When muscles contract during exercise, they release special signaling molecules called myokines. These molecules help regulate inflammation throughout the body.
Exercise also influences pathways involved in immune signaling and cellular repair. It can reduce harmful inflammatory cytokines while activating processes that support tissue regeneration.
In other words, movement does not only strengthen the muscle. It improves the cellular environment that allows muscle to stay healthy.
The most powerful approach combines both
Research consistently shows that the best outcomes occur when people combine:
Resistance exercise for strength
Aerobic activity for cardiovascular and metabolic health
Balance or stability work for coordination and fall prevention
Together these forms of movement support your nervous system, your muscle tissue, and your cellular repair systems that protect strength as you age.
The key message is simple
Muscle decline is not simply aging.
It is a biological process influenced by inflammation, inactivity, and reduced repair signals within muscle and nerve cells.
The encouraging truth is that the body continues to respond to movement throughout life:
Every walk.
Every strength session.
Every time you challenge your muscles.
You are never simply exercising.
With exercising, you are sending signals that help your body repair, rebuild, and protect muscle at the cellular level.
Reference:
Article reference:
Li, H., Chen, Z., & Songlin, X. (2026). Revitalizing Muscles: Harnessing Exercise to Modulate Inflammatory Cytokines and Conquer Sarcopenia in Aging. Cell Biochemistry and Biophysics. https://doi.org/10.1007/s12013-026-02004-4
Calcaterra, V., Vandoni, M., Rossi, V., Berardo, C., Grazi, R., Cordaro, E., et al. (2022). Use of physical activity and exercise to reduce inflammation in children and adolescents with obesity. International Journal of Environmental Research and Public Health, 19(11), 6908. https://doi.org/10.3390/ijerph19116908
Kunz, H. E., & Lanza, I. R. (2023). Age-associated inflammation and implications for skeletal muscle responses to exercise. Experimental Gerontology, 177, 112177. https://doi.org/10.1016/j.exger.2023.112177
Graff, R. M., Jennings, K., LaVoy, E. C., Warren, V. E., Macdonald, B. W., Park, Y., et al. (2022). T-cell counts in response to acute cardiorespiratory or resistance exercise in physically active or physically inactive older adults: A randomized crossover study. Journal of Applied Physiology, 133(1), 119–129. https://doi.org/10.1152/japplphysiol.00301.2021
Córdova, C., Lopes-e-Silva, J., Fernando, Pires, A. S., Souza, V. C., Brito, C. J., Moraes, C. F., et al. (2011). Long-term resistance training is associated with reduced Circulating levels of IL-6, IFN-gamma and TNF-alpha in elderly women. Neuroimmunomodulation, 18(3), 165–170. https://doi.org/10.1159/000323396
Antuña, E., Cachán-Vega, C., Bermejo-Millo, J. C., Potes, Y., Caballero, B., Vega-Naredo, I., et al. (2022). Inflammaging: Implications in sarcopenia. International Journal of Molecular Sciences, 23(23), 15039 https://doi.org/10.3390/ijms232315039
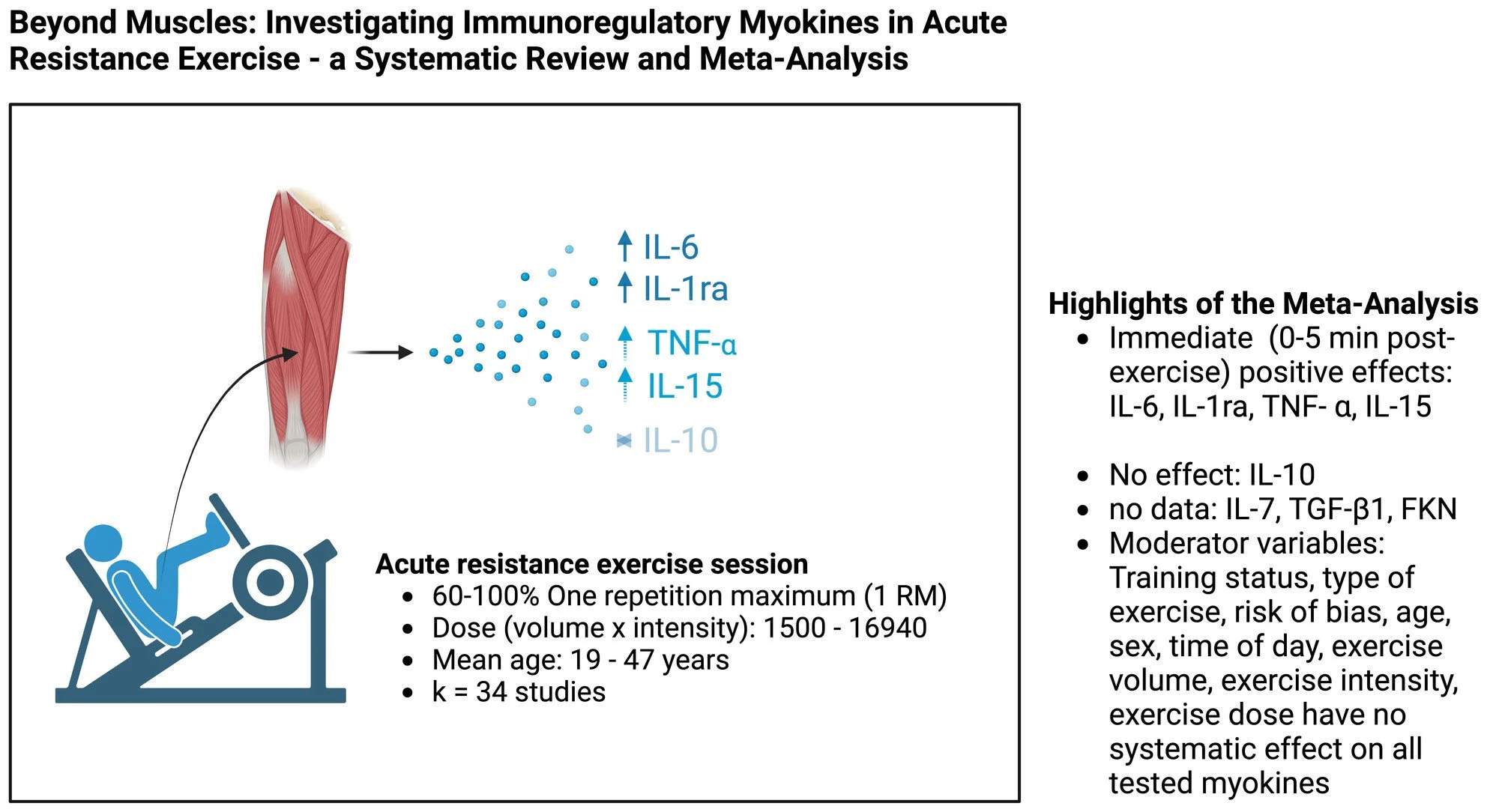
Ringleb, M., Javelle, F., Haunhorst, S., Bloch, W., Fennen, L., Baumgart, S., et al. (2024). Beyond muscles: Investigating immunoregulatory myokines in acute resistance exercise–A systematic review and meta-analysis. The FASEB Journal, 38(7), e23596 https://doi.org/10.1096/fj.202301619R
Shen, Y., Shi, Q., Nong, K., Li, S., Yue, J., Huang, J., et al. (2023). Exercise for sarcopenia in older people: A systematic review and network meta-analysis. Journal of Cachexia Sarcopenia and Muscle, 14(3), 1199–1211. https://doi.org/10.1002/jcsm.13225
Calcaterra, V., Vandoni, M., Rossi, V., Berardo, C., Grazi, R., Cordaro, E., et al. (2022). Use of physical activity and exercise to reduce inflammation in children and adolescents with obesity. International Journal of Environmental Research and Public Health, 19(11), 6908. https://doi.org/10.3390/ijerph19116908
Lee, H. S., & Lee, J. (2021). Effects of exercise interventions on weight, body mass index, lean body mass and accumulated visceral fat in overweight and obese individuals: A systematic review and meta-analysis of randomized controlled trials. International Journal of Environmental Research and Public Health, 18(5), 2635 https://doi.org/10.3390/ijerph18052635
Małkowska, P. (2024). Positive effects of physical activity on insulin signaling. Current Issues in Molecular Biology, 46(6), 5467–5487. https://doi.org/10.3390/cimb46060327
Bano, G., Trevisan, C., Carraro, S., Solmi, M., Luchini, C., Stubbs, B., et al. (2017). Inflammation and sarcopenia: A systematic review and meta-analysis. Maturitas, 96, 10–15. https://www.maturitas.org/article/S0378-5122(16)30342-5